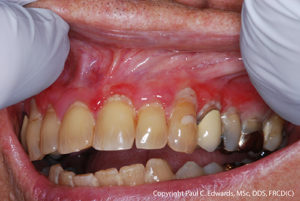
You can accelerate diagnosis times
Ask your patient:
- Do you have more than one blister or lesion in your mouth?
- Have your blisters or lesions lasted for more than a week?
- Have you continually had blisters or lesions that don’t heal?
- Do you have blisters or lesions in any locations outside the mouth?
If your patient answers YES to three or more of these questions, a biopsy should be considered. Both conventional H&E histology (in formalin) and DIF (in Michel’s/Zeus) are needed for a diagnosis. Specimens must contain intact epithelium over the underlying connective tissue.

Get your free information handout
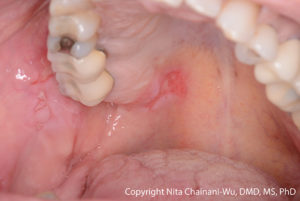
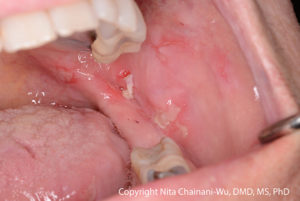
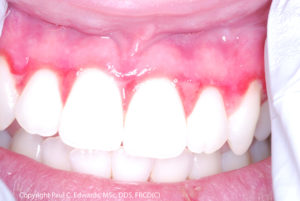
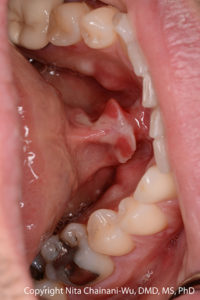
Clinical Presentation
Dental professionals should think of pemphigus vulgaris (PV) or mucous membrane pemphigoid (MMP) when there is a combination of:
- Multiple oral lesions
- Ulcerations preceded by bullae (however, in many cases, the bullae may not be evident to the patient or clinician)
- Chronic lesions (non-healing or very slow to heal)
- Primary lesions (lesion runs its course until resolved, as opposed to recurrent lesions, which come and go like cold or canker sores)
- Lesions may also occur outside of the mouth
A lesion can follow minor trauma. This is called a Nikolsky sign: cells pull apart and blister, and a lesion develops because the adhesion between cells is weakened.
The formation of a Nikolsky sign following minor lateral force on mucosa or gingiva can be a diagnostic aid. If a lesion develops, the patient almost certainly has PV or MMP. Patients can also experience “natural” Nikolsky phenomena: lesions following minor oral trauma (eating hard or sharp foods, etc.).
Biopsy Information
Accurate diagnosis of oral blistering diseases is predicated on obtaining a satisfactory biopsy for both hematoxylin and eosin (H&E) and direct immunofluorescence (DIF) evaluation. To be diagnostic, the biopsy specimens must contain intact epithelium over the underlying connective tissue. However, in the oral cavity these lesions are often fragile and separation between the epithelium and connective tissue is common, rendering the specimen non-diagnostic. A biopsy should be performed by a dentist or dental specialist experienced in performing biopsies of vesiculobullous lesions.
Here are some general guidelines:
- Do not sample the bed of an ulcer because there is no epithelium there, resulting in a non-specific diagnosis.
- As a general rule, biopsies must contain intact epithelium and should be taken from perilesional (within 1 cm) or normal appearing tissue rather than the directly ulcerated tissue because an ulcer, by definition, is missing the epithelium. Without the epithelium, it is not possible to detect destruction between epithelial cells (as in PV) or between epithelial cells and the underlying connective tissue (as in MMP).
- During the biopsy procedure, avoid any action that may cause separation of the epithelium from underlying connective tissue, e.g. rubbing the area with gauze to remove saliva or blood.
- Two specimens must be taken with samples submitted for BOTH routine hematoxylin and eosin (H&E) stain (storing specimen in 10% formalin) AND for direct immunofluorescence testing (MUST submit sample in Michel’s transport medium and send to pathology laboratory as quickly as possible to preserve antibody detection).
- When performing DIF biopsies, have Michel’s solution on hand. If planning to perform DIF biopsies, order and store in advance the Michel’s transport medium. Identify IN ADVANCE a commercial laboratory equipped to perform DIF studies.